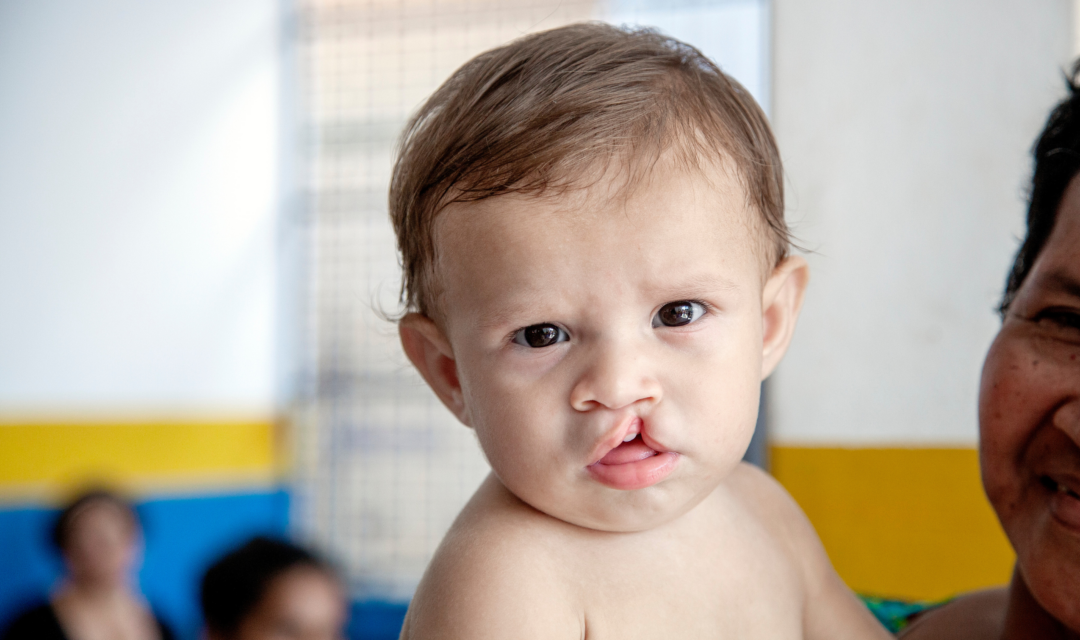
Save the life of a child like Fredy
Babies born with a cleft are nine times more likely to die before their first birthday. With your help we can change this statistic and provide life-saving surgery and cleft care.
Your support can change the lives of thousands of children like Joseph who are waiting for their new smiles.

What is a cleft condition?
A cleft condition is a gap in the mouth that didn’t close during the early stages of pregnancy. Worldwide, it’s estimated that a child is born every three minutes with a cleft lip or cleft palate, that’s one in every 500 – 700 births.

Cleft care and support
Cleft surgery can transform a child’s life, but our patients often need the care of many different specialists during their journey. Operation Smile teams provide the full package of support, from nutrition, dentistry and orthodontic to speech therapy and psychosocial care.

Get involved
Partner with us
We partner with leading organisations in Ireland – join us and be a force for good.
Leave a gift in your will
Remember Operation Smile in your will and have a lasting impact on children with cleft conditions around the world.
Where we work
 Find out more about our work in
Find out more about our work in A smile in your inbox


