
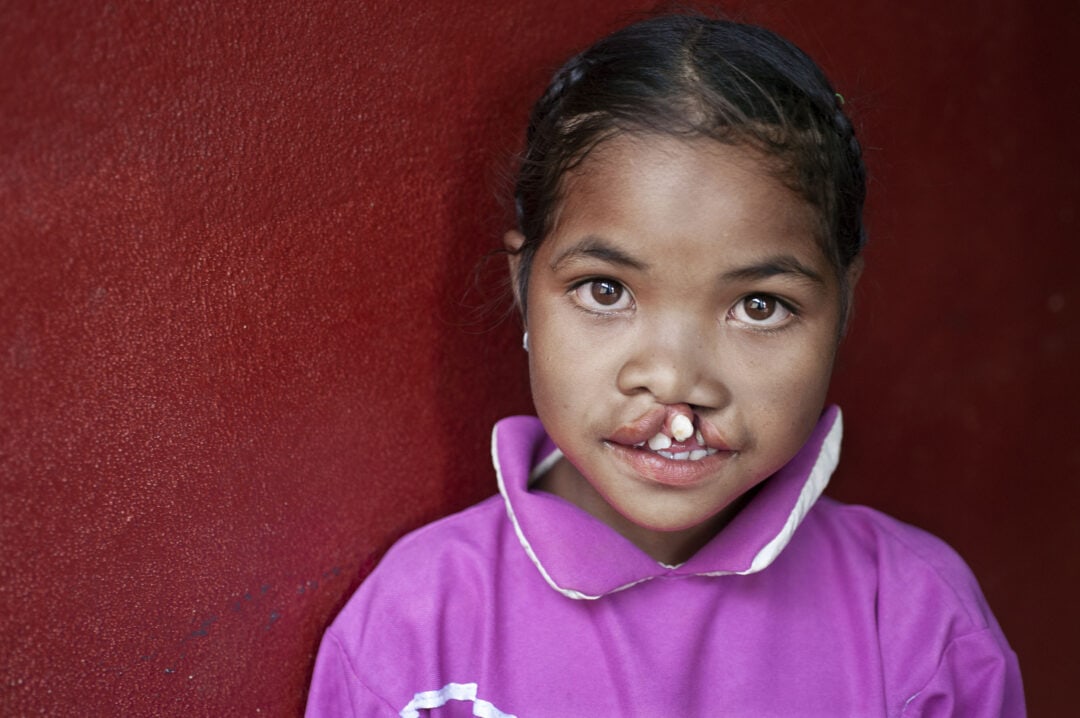
Inspiring stories

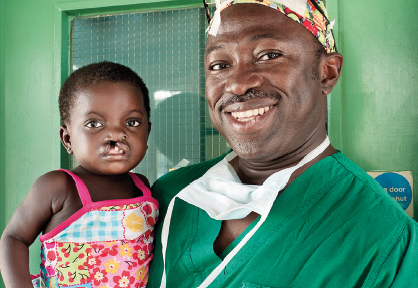



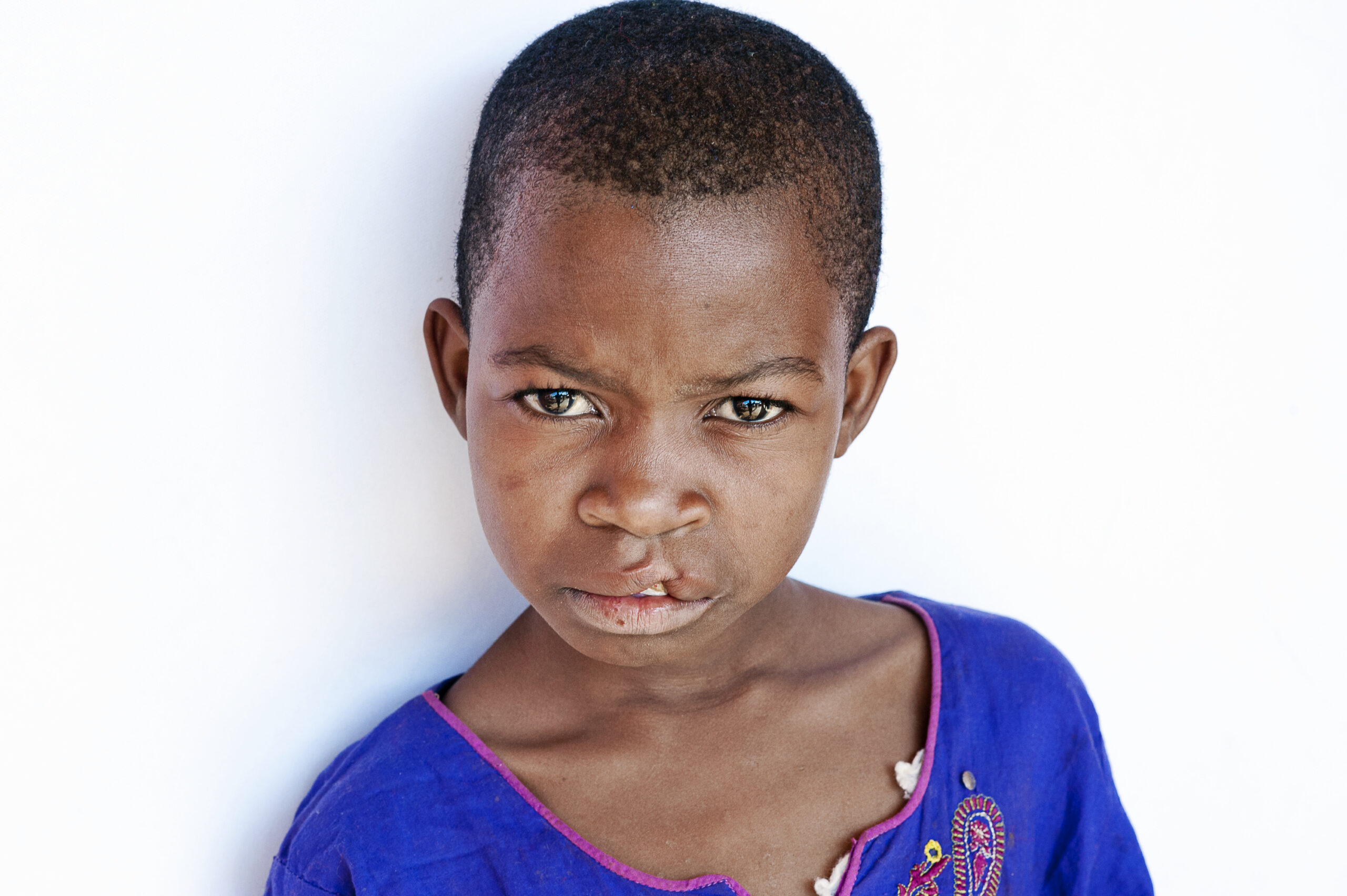



Programme updates
Find out how our surgical programmes are strengthening local health systems and training the next generation of medical leaders.
Training anaesthetists in Rwanda
Anaesthesia is vital to the delivery of safe surgery, but there is a dramatic shortage of trained anaesthetists in Rwanda. In this densely popualated country, 11.9 million people are served by just 15 anaesthetists and anaesthesiologists.
Dr Paulin Banguti is working to fill this void – he’s director of the post-graduate anaesthesia programme at the University of Rwanda. During the March 2016 Operation Smile surgical training rotation at Rwinkwavu District Hospital, he led a group of anaesthesia residents to observe and learn from volunteer anaesthesiologists from around the world.
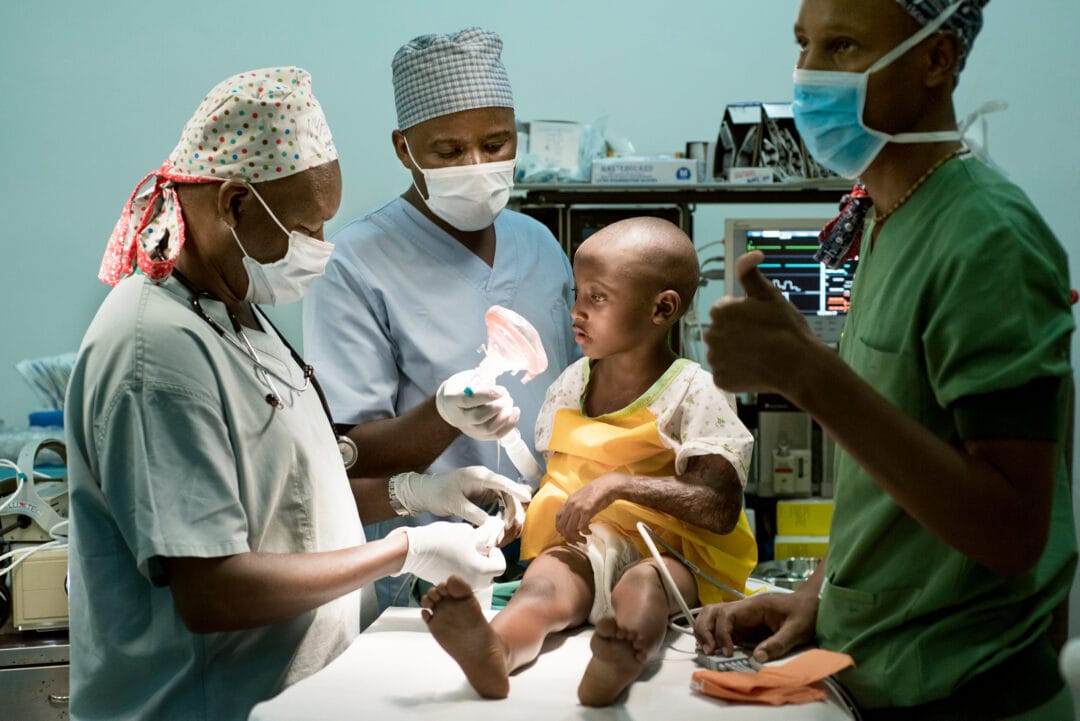
Strengthening health systems in Malawi
To enable Operation Smile to serve and treat more people living with cleft conditions, we focus on increasing the surgical capacity of low-and middle-income countries like Malawi so that cleft care for local people can continue, even after a surgical programme ends.
Operation Smile Malawi has worked to encourage and educate local surgeons, doctors and nurses, and now has nearly 50 percent of its medical volunteers from Malawi. Surgical training rotations train and empower local surgeons to help their own communities and strengthen health systems for the future.
